AI in Public Health: Modernizing Government Health Systems
The way governments deliver healthcare is undergoing a seismic shift. Across the globe, public health agencies are grappling with aging populations, escalating chronic disease burdens, widening health disparities, and the ever-present threat of emerging infectious diseases. Against this backdrop, AI in public health has moved from a speculative technology to a practical, mission-critical tool.
Government health agencies are now investing in AI not as a luxury, but as a strategic necessity. From predictive disease surveillance to AI-powered care coordination platforms, artificial intelligence is enabling health systems to do more with less responding faster, serving broader populations, and making smarter decisions grounded in real-time data.
This post examines why governments are embracing AI, what practical applications are driving results today, and how health agencies can build a scalable, responsible path toward AI-enabled modernization.
Why Governments Are Turning to AI in Public Health
Public health systems have long operated under pressure: fragmented data silos, underfunded infrastructure, slow bureaucratic response cycles, and a widening gap between population need and available resources. Traditional approaches to disease surveillance, care coordination, and health policy have struggled to keep pace with the complexity of modern health challenges.
Digital transformation for government is now the driving mandate, and AI sits at its core. Here is why the urgency is real:
- Fragmented data ecosystems make it nearly impossible to get a unified view of population health. Patient records span dozens of disparate systems, often incompatible with one another.
- Resource constraints mean that public health agencies must stretch every dollar. Manual processes for reporting, case management, and outreach are labor-intensive and error-prone.
- Slow response times during health crises from COVID-19 to mpox outbreaks revealed that reactive, siloed public health systems are dangerously insufficient.
AI addresses these structural weaknesses by enabling predictive analytics, automating administrative workflows, and giving decision-makers access to actionable intelligence at scale. When paired with thoughtful digital transformation for government strategy, AI doesn’t just improve efficiency it fundamentally reimagines what public health delivery can look like.
Key AI Applications in Public Health
Predictive Analytics for Disease Surveillance
One of the most powerful AI applications in public health is predictive surveillance. Machine learning models can analyze patterns across environmental data, social determinants, demographic trends, and historical case data to forecast where outbreaks are likely to emerge days or even weeks before traditional surveillance methods would detect them.
The CDC’s use of AI-enhanced flu surveillance systems is a well-documented example. By integrating emergency department visit data with social media signals and climate indicators, these models have demonstrated the ability to predict flu season peaks with significantly higher accuracy than baseline approaches.
AI-Driven Patient Monitoring Through Digital Health Platforms
Digital Health Platforms are transforming how government agencies monitor and engage patients between clinical touchpoints. AI-powered platforms can flag patients at high risk of hospitalization, automate check-in workflows, and surface care gaps in real time enabling care teams to prioritize outreach proactively rather than reactively.
For patients managing chronic conditions such as diabetes, hypertension, or HIV, this continuous intelligence layer is life-changing. It shifts the care model from episodic and reactive to continuous and preventive.
The Ryan White HIV Platform: AI in Action for Care Coordination
A compelling illustration of AI applied to a government-mandated health program is found in the evolution of HIV care management infrastructure. The Ryan White HIV Platform which supports care services for low-income individuals living with HIV under the Ryan White HIV/AIDS Program is increasingly leveraging AI and data analytics to drive care coordination and improve patient outcomes.
By integrating AI capabilities into Ryan White client management systems, health agencies and their technology partners can identify clients who have fallen out of care, predict which patients are at highest risk of viral non-suppression, and automate appointment reminders and medication adherence outreach. These capabilities directly support the national goal of ending the HIV epidemic by improving retention in care and treatment outcomes across historically underserved populations.
Generative AI Use Cases in Healthcare
Generative AI use cases in healthcare are rapidly expanding beyond the experimental stage. Government health agencies are beginning to use large language models to:
- Draft and localize health education materials across multiple languages and literacy levels
- Support public health researchers by synthesizing vast literature reviews in hours rather than weeks
- Generate first drafts of policy briefs and public communications during health emergencies
- Assist clinicians in navigating complex clinical guidelines with natural language queries
These applications reduce administrative burden and free up human expertise for higher-order tasks.
AI in Universities for Workforce Development and Research
AI use in universities is producing the next generation of public health practitioners equipped to work in AI-enabled environments. Schools of public health at institutions like Johns Hopkins, Harvard, and University of Washington have embedded AI and data science coursework directly into their public health curricula.
Beyond training, university research centers are partnering with state and federal health agencies to develop and validate AI models for population health management, health equity analysis, and epidemiological forecasting creating a virtuous cycle between research innovation and real-world deployment.
How Government AI Consulting Supports Public Health Modernization
Integrating AI into a government health system is not simply a technology project it is an organizational transformation. This is where government AI consulting plays an indispensable role.
Experienced consulting partners help agencies navigate the complex intersection of technology, policy, and operations. Specifically, they support:
- Strategic roadmapping: Identifying which AI use cases will deliver the highest public health impact given existing infrastructure and data assets.
- Compliance and governance: Ensuring AI implementations align with HIPAA, 42 CFR Part 2, and other federal and state regulatory frameworks governing health data.
- Systems integration: Bridging the gap between new AI tools and existing legacy platforms, including Electronic Health Records (EHRs), case management systems, and benefits administration platforms.
- Change management: Preparing the public health workforce to adopt AI-enhanced workflows through training, communication, and process redesign.
Without this level of strategic support, even well-funded AI initiatives can stall at the pilot stage. Government AI consulting provides the institutional knowledge and implementation expertise needed to scale solutions responsibly and sustainably.
Benefits and Outcomes of AI in Government Health Systems
The return on investment from AI in public health is measurable and growing. Agencies that have moved beyond experimentation and into scaled deployment are reporting:
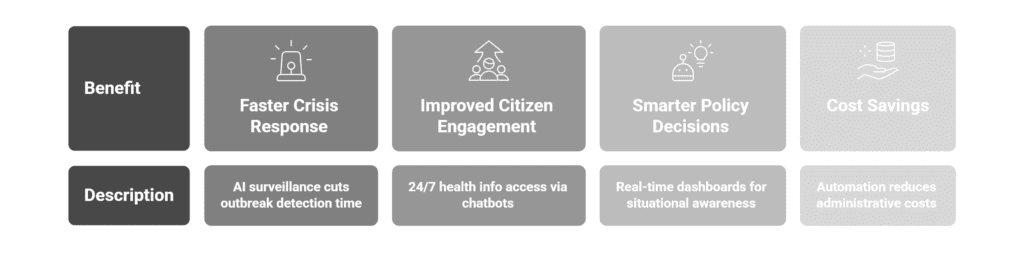
- Faster crisis response: AI-powered surveillance systems cut outbreak detection time from weeks to days, enabling earlier containment measures.
- Improved citizen engagement: AI-powered chatbots and digital platforms deliver 24/7 health information access, reducing call center load and improving satisfaction scores.
- Smarter policy decisions: Real-time dashboards powered by AI give health officials the situational awareness needed to allocate resources, target interventions, and evaluate program effectiveness with unprecedented precision.
- Cost savings: Automating eligibility determinations, appointment scheduling, and case documentation generates measurable administrative cost reductions often in the range of 20–40% for targeted processes.
Challenges and Considerations
Responsible deployment of AI in government health systems requires clear-eyed acknowledgment of the challenges involved.
Algorithmic bias is among the most serious concerns. AI models trained on historically inequitable datasets risk perpetuating or amplifying disparities in care particularly for Black, Indigenous, and other marginalized communities. Rigorous model auditing and diverse training data are non-negotiable requirements.
Data privacy and cybersecurity remain paramount. Public trust in government health systems depends on the secure handling of sensitive health information. Any AI deployment must incorporate robust data governance frameworks, role-based access controls, and regular security audits.
Legacy system integration presents persistent technical challenges. Many government health agencies operate on infrastructure that is decades old and not designed for modern data exchange. API-based integration strategies and phased modernization roadmaps are typically required.
Workforce readiness is perhaps the most underestimated barrier. AI tools are only as effective as the people using them. Investment in AI literacy training, change management, and collaborative design with frontline health workers is essential to sustainable adoption.
Real-World Examples and Case Studies
New York City Department of Health deployed an AI-driven syndromic surveillance system that monitors emergency department data in near real-time, enabling health officials to detect anomalous disease patterns within hours of emerging trends a capability that proved invaluable during COVID-19 surge monitoring.
The Ryan White HIV Platform, as implemented in multiple state health departments, has demonstrated measurable improvements in viral suppression rates when AI-driven care gap identification is integrated into case management workflows. Clients identified by predictive models as at-risk for falling out of care showed significantly higher re-engagement rates when proactive outreach was triggered automatically.
University of Pittsburgh’s Public Health Dynamics Laboratory partnered with county and state health agencies to deploy AI-based models for predicting opioid overdose hotspots, enabling targeted naloxone distribution and harm reduction resource deployment resulting in documented reductions in overdose mortality in pilot counties.
These examples demonstrate that AI, when implemented with strong data governance, clear use case definition, and stakeholder engagement, delivers real and measurable improvements in public health outcomes.
Best Practices for Implementing AI in Public Health
For government health leaders ready to move from strategy to execution, these practices consistently distinguish successful implementations from stalled pilots:
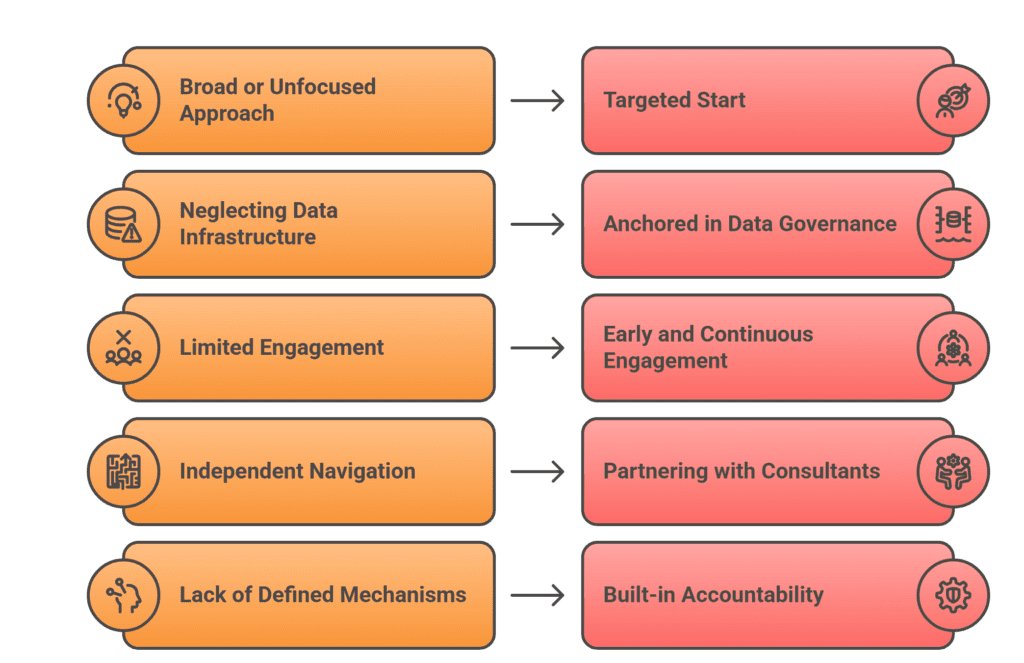
- Start targeted. Select one high-impact use case care gap identification, disease surveillance, or benefits eligibility and build a time-bound pilot with defined success metrics before scaling.
- Anchor in data governance. AI is only as good as the data feeding it. Invest in data quality, standardization, and interoperability infrastructure before expecting AI to deliver results.
- Engage stakeholders early and continuously. Policymakers, frontline health workers, community advocates, and patients all have critical perspectives that should shape AI design. Co-design processes lead to better adoption and more equitable outcomes.
- Partner with experienced government AI consultants. Navigate procurement, compliance, and integration complexity with partners who understand the unique constraints of public sector health technology.
- Build in accountability mechanisms. Define model performance benchmarks, establish regular bias audits, and create clear escalation paths for when AI recommendations conflict with clinical or community knowledge.
Future Trends: The Next Wave of AI in Public Health
The trajectory of AI in public health points toward even more transformative capabilities in the years ahead:
Generative AI will scale health communications. As generative AI use cases in healthcare mature, agencies will deploy AI to produce tailored health guidance, crisis communications, and community education materials at a speed and personalization level previously impossible.
IoT and wearable integration will enable continuous population health monitoring. Connected devices from glucometers to air quality sensors will feed real-time data into AI systems that can detect emerging health risks at both the individual and community level.
Predictive policymaking will become a practical reality. AI models will help health officials simulate the downstream impact of policy interventions from tobacco tax increases to housing investment before implementation, enabling smarter resource allocation and health equity planning.
The use of AI in these contexts will not replace the human judgment that defines good public health leadership. But it will dramatically expand the capacity of public health systems to see clearly, act quickly, and serve equitably.
Conclusion: AI as a Catalyst for Modern Government Health Systems
The case for AI in public health is no longer theoretical. From predictive surveillance and the Ryan White HIV Platform to generative AI-powered health education and AI-driven Digital Health Platforms, the technology is delivering real results in government health systems today.
What separates health agencies that realize these benefits from those that remain stuck in pilot purgatory is not access to technology it is strategic intent, stakeholder alignment, and expert implementation support. By partnering with experienced government AI consulting firms, committing to strong data governance, and investing in workforce readiness, government health agencies can move from experimentation to transformation.
The future of public health is intelligent, data-driven, and deeply human. AI is the tool that makes that future possible. The time to invest thoughtfully, boldly, and equitably is now.
Frequently Asked Questions
What are common AI applications in public health?
AI is used for disease surveillance, outbreak prediction, and health data analysis. For example, AI models forecast disease spread and power chatbots for health guidance. These tools help agencies respond faster to health trends.
How do governments benefit from AI in health?
AI enables better decision-making with big data. Governments can use AI to allocate resources (like vaccines or staff) more efficiently and personalize health messaging. Automated AI tools save time on reporting and allow staff to focus on care.
What are the risks of AI in public health?
Key risks include data privacy and bias. Health data is sensitive, so strong security is vital. Also, if training data isn’t diverse, AI could give inaccurate results for some groups. Governments must enforce standards and audits to prevent misuse or unfair outcomes.
Can you give examples of AI in action now?
Yes. For instance, during COVID-19, agencies used AI to analyze X-rays and forecast cases. Health departments employ AI dashboards to spot infection clusters. Universities use AI chatbots to train students in outbreak response. These cases show AI boosting both practice and education in public health.
How do governments ensure ethical AI use?
They establish guidelines and oversight. Agencies appoint AI ethics boards and require human review for high-impact AI systems. Training programs help officials learn about AI governance. The aim is to balance innovation with transparency and trust.
How does AI affect health workforce skills?
Many agencies now train staff in data science and AI. Employees learn to work with AI tools and to interpret their outputs. Academic partnerships (like joint programs with universities) also prepare future public health workers to use AI responsibly. This ensures technology aids rather than replaces human expertise.






